Spring 2023 - Vol. 18, No. 1
PHOTO QUIZ FROM URGENT CARE
A Late-Term Pregnant Female with Ear Pain
Zachary Jupin, PA-C
Physician Assistant
Penn Medicine Lancaster General Health Urgent Care
CASE HISTORY
A 32-year-old non-smoking female who is 39 weeks gestation presents complaining of ear pain, pruritus, and decreased hearing in the left ear for the past two days. She denies tinnitus, vertigo, otorrhea, headaches, fevers, symptoms of a urinary tract infection, or problems with the right ear. She denies any recent antibiotic or corticosteroid use. She is nondiabetic. There was no reported recent swimming.
EXAM
The left ear canal is edematous with a white purulent collection and black budding spores (see Fig. 1). The tympanic membrane cannot be visualized. There is no external erythema or swelling. There is mildly tender posterior auricular lymphadenopathy.
QUESTIONS
1. What is the cause of this patient’s ear pain, and what are the most common offending pathogens?
2. What are some risk factors for developing this infection?
3. What are the most appropriate next steps for this patient?
4. What are potential complications if left untreated?
ANSWERS
1. Fungal otitis externa/otomycosis is commonly caused by Aspergillus and Candida.
2. Risk factors include type 2 diabetes mellitus, recent corticosteroid or antibiotic use
(particularly fluoroquinolone drops), history of immunosuppression, humid climate,
recent instrumentation of ear, and use of hearing aids.1
3. Next steps might include one or more of the following:
a. Once or twice daily debridement or flushing of the ear canal.
b. Treatment with local or systemic antifungal agents.
c. Discontinuation, if appropriate, of any unnecessary agents.
d. Appropriate management of any chronic medical disorders.
e. Discontinuation or appropriate cleaning of any hearing aids or other ear protection/listening devices.
f. Consideration of ENT referral for refractory cases.
4. Complications may include serous otitis media (30% of patients), tympanic membrane perforation (15%),
and external auditory canal osteitis (5%).2
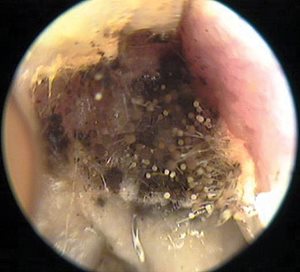
Fig. 1. Ear canal with white purulent collection and black budding spores.
Photo by Kevin Kavanagh, MD. Used with permission.
DISCUSSION
Otomycosis is a superficial mycotic infection of the outer ear canal that can usually be diagnosed clinically by direct examination of the ear in conjunction with reported symptoms. The mycosis results in inflammation, swelling, and superficial epithelial masses of debris containing hyphae and suppuration. Pruritus has been frequently cited as one of the hallmark symptoms, present in up to 93% of cases, followed closely by hearing loss and aural fullness, which are the result of accumulation of fungal debris in the canal.3
Aspergillus and Candida species are the most identified fungal pathogens in otomycosis. Aspergillus reveals a characteristic black dots debris, but infection with Candida can be more difficult to detect clinically because of its lack of a characteristic appearance; it can present as otorrhea not responding to aural antimicrobial. Otomycosis attributed to Candida can be identified by culture data.4
Multiple studies have examined the efficacy of various antifungal agents, however there is no consensus on the most effective agent. Topical 1% clotrimazole seems to be the preferred antifungal medication for its action against both Aspergillus and Candida species. Salicylic acid (2%) in alcohol has also been used but seems less effective. Oral fluconazole may be considered but carries greater risk of side effects, including hepatotoxicity.5,6
Application of appropriate topical antifungal agents coupled with frequent mechanical debridement usually results in prompt resolution of symptoms, although recurrent or residual disease can be common. Duration of treatment may vary, but most patients have resolution of infection within two weeks. Refractory cases should be referred to ENT.
REFERENCES
1. Osguthorpe JD, Nielsen DR. Otitis externa: review and clinical update. Am Fam Physician. 2006;74(9):1510-1516.
2. Anwar K, Gohar MS. Otomycosis; clinical features, predisposing factors, and treatment implications. Pak J Med Sci. 2014;30(3):564-567.
3. Pradhan B, Tuladhar NR, Amatya RM. Prevalence of otomycosis in outpatient department of otolaryngology in Tribhuvan University Teaching Hospital, Kathmandu, Nepal. Ann Otol Rhinol Laryngol. 2003;112(4):384-387.
4. Vennewald I, Klemm E. Otomycosis: diagnosis and treatment. Clin Dermatol. 2010;28(2):202-211.
5. Navaneethan N, YaadhavaKrishnan RP. Type of antifungals: does it matter in empirical treatment of otomycosis? Indian J Otolaryngol Head Neck Surg. 2015;67(1):64-67.
6. Munguia R, Daniel SJ. Ototopical antifungals and otomycosis: a review. Int J Pediatr Otorhinolaryngol. 2008;72(4):453-459.