 Click to Print Adobe PDF
Click to Print Adobe PDF
|
Fall 2010 - Vol.5, No.3
Progress in the Management of Sepsis
Joseph M. Kontra, M.D.
Infection Specialists of Lancaster
|
 |
An intensive, multi-disciplinary project to reduce sepsis mortality by the application of evidence-based guidelines was initiated at LGH in 2007. This paper reports on the progress of that initiative.
The Surviving Sepsis Campaign
In 2004 the Surviving Sepsis Campaign (SSC), an international group of experts representing 11 academic organizations, published the first clinical guidelines for the comprehensive management of severe sepsis and septic shock.1 They defined a Sepsis Resuscitation Bundle (SRB) that was designed for implementation in the critical first 6 hours of the diagnosis. Key components of the SRB include:
1. Measure serum lactate
2. Obtain blood cultures prior to antibiotic administration
3. Administer broad spectrum antibiotics within one hour
4. Deliver initial fluid bolus of 1L crystalloid
5. Maintain central venous pressure of > 8mm Hg
6. Apply vasopressors to achieve mean arterial pressure of >65 mm Hg
7. Achieve central venous O2 saturation of > 70%
Also included in the SSC recommendations was a Sepsis Management Bundle (SMB), which detailed guidelines for the management of patients in the first 24 hours. Components of the SMB included:
1. Low-dose steroid administration per ICU policy
2. Drotrecogin alpha administration per ICU policy
3. Glucose control protocol
4. Ventilator protocol to limit peak pressures
In 2006, this Journal published plans for application of the guidelines at LGH.2 Subsequent updates to the original guidelines were published by SSC in 2008,3 and were incorporated into the LGH sepsis project as well. With strong board and administrative support, a multi-departmental, multi-disciplinary project was launched with the ultimate intent of reducing the high mortality associated with severe sepsis and septic shock by adherence to the SSC guidelines. Sepsis management became a priority initiative for Quality Improvement at LGH.
International Experience and Benchmarking
Timely application of all 11 components of the SSC recommendations proved to be more difficult in the real world of hospital practice than in the medical research centers where they were forged. Process improvement initiatives designed to change well-entrenched clinical behaviors were both time-consuming and difficult. Collection and processing of data were tedious. The project required many modifications in hospital infrastructure. In addition, variations in the details of guideline implementation from hospital to hospital made benchmarking problematic. Nonetheless, with much trepidation steady progress seemed to follow. Earlier this year, SSC published the results of its own international performance improvement program which finally provided meaningful benchmarking data.4 The analysis included 15,022 patients in 165 hospitals from the U.S., Europe, and South America, studied from January 2005 through March 2008. Compliance with the entire SSC sepsis management bundle was only 18.4% in the first quarter of the study, but it increased to 36.1 % by the end of the 2-year study. Mortality decreased from 37% to 30% during the same period.
Results at Lancaster General Hospital
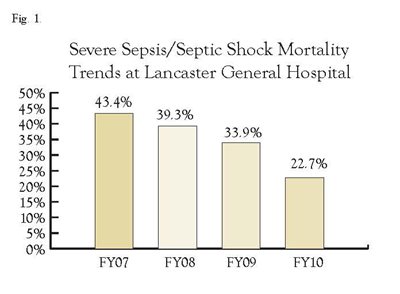
From fiscal year 2007 through 2010, the mortality from severe sepsis and septic shock at LGH declined steadily from 43.4% to 22.7% (See Fig.1). This represented a 48% reduction in crude mortality during the 4-year project. This also compares favorably to the 95th percentile of mortality in the MIDAS (Medical Information Database Access System) database. Overall, compliance with all components of the sepsis bundle increased from approximately 15% to 31% during the study period, similar to the SCC international data.
Future Directions
The greatest challenge in implementation of the SSC guidelines remains the first 6 hours of management, during which a timely diagnosis and prompt initiation of the aggressive SRB is critical. Through collaboration with the medical staff, a pilot program was launched in July 2010 utilizing physicians with Board Certification in critical care as the admitting physicians for all emergency department sepsis admissions. Continuous study and refinement of the management of severe sepsis and septic shock will hopefully foster progressive reduction in mortality in these critically ill patients.
REFERENCES
1 Dellinger RP, Carlet JM, Masur H, et al. Surviving Sepsis Campaign guidelines for management of severe sepsis and septic shock. Critical Care Medicine. 2004;32(3):858-873.
2 Kontra, JM. Evidence-Based Management of Severe Sepsis and Septic Shock. J Lanc Gen Hosp. 2006;1(2):39-46.
3 Dellinger RP, Levy MM, Carlet JM, et al. Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock: 2008. Intensive Care Medicine. 2008 Jan;36(1):296-327.
4 Levy, MM, et al. The Surviving Sepsis Campaign: Results of an international guideline-based performance improvement program targeting severe sepsis. Critical Care Medicine. 2010; 38:367-74.