Fall 2022 - Vol. 17, No. 2
SCIENTIFIC REPORT
Syphilis: A Review
Carr Reese Cox Siegel
Patricia Carr Reese, MD, MPH, AAHIVS
Family Physician
LG Health Physicians Comprehensive Care
Julie Cox, MD
Gabrielle B. Siegel, MD
Family Physicians, Family Medicine Residency Program
Penn Medicine Lancaster General Health
Sir William Osler’s aphorism “to know syphilis is to know medicine” still holds true in the year 2022 as the syphilis epidemic continues. As sexual practices and behaviors change, syphilis cases in Pennsylvania are at the highest they have been in the last 30 years.
1 In light of the recent increase in cases, this article aims to review the diagnosis, treatment, and screening guidelines for syphilis, with a particular focus on two key groups: men who have sex with men, and women of reproductive age.
EPIDEMIOLOGY
In 1999, the Centers for Disease Control and Prevention (CDC) initiated a campaign to eradicate syphilis when rates were at an all-time low. Unfortunately, this was unsuccessful: rates began to increase after 2000 and have escalated further in the recent past.
2 Per CDC Sexually Transmitted Disease (STD) Surveillance 2019 data, 41% of the cases of primary and secondary syphilis occur among men who have sex with men (MSM), followed by men who have sex with women (MSW) (18%) or unknown sexual partners (17%), women (16%), and finally, men who have sex with men and women (5%).
3
Updated data demonstrate a dramatic increase in incident cases of primary and secondary syphilis among women (see Fig. 1).
4 A primary driver of this increase is methamphetamine use and an associated sexual disinhibition (referred to as “ChemSex”) and needle sharing (see Fig. 2). Unfortunately, with the increased incidence of syphilis comes the rise of syphilis in the pregnant population and subsequently increased cases of congenital disease.
3

Fig. 1. Primary and secondary syphilis, reported cases by sex and sex of sex partners, United States, 2016-2020 (includes men having sex with unknown sex of sex partners, MSU).4
 Fig. 2. Reported* injection drug use, methamphetamine use, heroin use, and sex with a person who injects drugs (PWID) among primary and secondary syphilis cases, United States, 2015-2019.4 (*Proportion reporting each factor with the last 12 months calculated among cases with known data (cases with missing or unknown responses excluded from denominator.)
Fig. 2. Reported* injection drug use, methamphetamine use, heroin use, and sex with a person who injects drugs (PWID) among primary and secondary syphilis cases, United States, 2015-2019.4 (*Proportion reporting each factor with the last 12 months calculated among cases with known data (cases with missing or unknown responses excluded from denominator.)
Over the last year in Pennsylvania, syphilis cases increased 28% with the highest number of early syphilis cases seen in the past 30 years, prompting changes in screening recommendations detailed below.
1 Data from the Sexually Transmitted Diseases Clinic at Lancaster General Health Physicians Comprehensive Care document high rates of syphilis infection in our own community (see Fig. 3).
5 Between November 2020 and November 2021, the clinic saw 54 cases of syphilis, which compares to only 35 cases in all of Lancaster County in 2019.
 Fig. 3. STDs found over time at LGHP Comprehensive Care Sexually Transmitted Diseases Clinic using chlamydia (CT) and gonorrhea (GC) lab testing.5
NATURAL HISTORY
Treponema pallidum (T. pallidum)
Fig. 3. STDs found over time at LGHP Comprehensive Care Sexually Transmitted Diseases Clinic using chlamydia (CT) and gonorrhea (GC) lab testing.5
NATURAL HISTORY
Treponema pallidum (T. pallidum) is the infectious agent that causes syphilis.
6 Known as the great imitator, syphilis can be difficult to diagnose as it takes different forms throughout the course of the disease. This is complicated by the fact that while the early stages of the disease are symptomatic, later stages of the disease are primarily asymptomatic.
Syphilis is spread via sexual or vertical transmission. Untreated, it progresses through primary, secondary, latent, and tertiary phases (see Fig. 4).
6 These phases can overlap, especially in persons living with HIV/AIDS (PLWHA). Of note, neurosyphilis, otosyphilis, and ocular syphilis can be present during any phase.
 Fig. 4. The natural history of untreated syphilis. Source: New York City Department of Health and Mental Hygiene, and New York City STD Prevention Training Center. Used with permission.
Fig. 4. The natural history of untreated syphilis. Source: New York City Department of Health and Mental Hygiene, and New York City STD Prevention Training Center. Used with permission.
In the context of sexual transmission, the chancre of primary syphilis occurs at the site of inoculation and is the manifestation of local spirochete infection. Classical teaching suggests that chancres associated with syphilis are single, sharply demarcated, painless ulcers; however, at least 30% of the time patients have multiple, painful ulcers (see Fig. 5a).
6 This is more common among PLWHA.

Fig. 5a. Ulceration on the upper lip of a patient with primary syphilis.7
Chancres may be hidden in places such as the cervix or rectum, or there may be no chancre at all. The latter is more common with reinfection. The chancre appears within the first 90 days of exposure, with median appearance at day 21. Chancres heal spontaneously within one to six weeks even without treatment, which often delays presentation to care.
Untreated individuals experience symptoms of secondary syphilis four to eight weeks after resolution of primary symptoms. While primary syphilis is a product of local infection, secondary syphilis is a product of systemic dissemination. Although symptoms are delayed, systemic dissemination begins within hours to days of inoculation, demonstrated by the fact that spirochetes can be found in the central nervous system by that time.
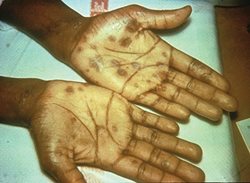
A wide variety of symptoms occur in secondary syphilis. Symptoms may be nondescript and generalized such as fever, headache, anorexia, myalgias, and adenopathy. Rashes are common and can take on almost any character, including being macular, papular, annular, psoriasiform, and rarely necrotic (see Fig. 5b). Rashes on palms and soles of the feet always warrant syphilis testing (see Fig. 5c).
6 Other skin/mucous membrane complications include mucous patches in the mouth, condyloma lata, and “moth eaten” alopecia.

Fig. 5b. Rash on the arms of a patient with secondary syphilis.
Syphilis can further cause gastritis, transaminitis (with alkaline phosphatase elevation out of proportion to alanine aminotransferase/aspartate aminotransferase), proctitis (similar in appearance to inflammatory bowel disease on biopsy), glomerulonephritis, nephrotic syndrome, and arthritis.
Without treatment, symptoms of secondary syphilis will also self-resolve. At this point in time, the infection is asymptomatic or “latent.” Latent syphilis is divided into early latent and late latent, the latter term describing infection that has lasted more than one year and is rarely transmissible.
Tertiary syphilis occurs years to decades after initial infection and can produce a variety of morbidities, including: cardiovascular disease such as aortic aneurysms, aortic valve insufficiency, and myocarditis; neurological complications including ataxia from Tabes dorsalis; and gumma of skin, bone, viscera, and soft tissues. Although frequently noted in the pre-antibiotic era, these presentations are not commonly seen since the discovery of antibiotics.
Neurosyphilis is further classified into early or late forms, which are distinguished by whether the disease has affected the meninges and vasculature (early) or has disseminated into the spinal cord parenchyma. Symptoms of acute syphilitic meningitis may include headache, confusion, or cranial nerve abnormalities, while meningo-vascular syphilis may present as a stroke-like syndrome and potentially progress to stroke due to inflammatory occlusion of vessels.
Late neurosyphilis is a presentation of tertiary syphilis. Ocular syphilis most commonly causes uveitis, and patients will often report diminished visual acuity. Otosyphilis affects hearing and balance.
DIAGNOSIS
The key to diagnosis of syphilis is a low threshold to include syphilis in the differential diagnosis and a thorough clinical history, including a sexual history. A good sexual history can be guided by the CDC’s five Ps:
Partners,
Pregnancy,
Protection from sexually transmitted infections (STIs), sexual
Practices, and
Past history of STIs.
Two general categories of serological testing are treponemal and nontreponemal. Treponemal tests include EIA, CIA, TP-PA, and FTA-ABS, which all refer to assays that detect
T. pallidum antibodies. Nontreponemal tests, such as rapid plasma reagin (RPR) and venereal disease research laboratory (VDRL), detect anti-cardiolipin antibodies present in individuals with syphilis.
Treponemal testing is increasingly being performed as the initial screening test for syphilis, followed by nontreponemal testing for confirmation. This method of testing is the “reverse sequence” algorithm and is more cost effective than the “traditional sequence algorithm,” which uses nontreponemal immunoassay as the screening test and treponemal assay as the confirmatory test (see Fig. 6).
6

In many cases, once an individual is exposed to syphilis, treponemal assays will remain positive regard. Less of treatment status. Nontreponemal assays are utilized to document treatment success and identify reinfection. The most common nontreponemal assays are RPR and VDRL. It is important to note that these are not interchangeable when assessing treatment success or reinfection; an RPR titer can only be compared to an RPR titer.
Treatment success is assured by at least a fourfold decrease in the nontreponemal titer (see Fig. 7).
6 This may take months or even up to two years to occur, so it is important in non-pregnant patients to delay repeat testing for at least three to six months to avoid unnecessary re-treatment or patient distress regarding reinfection. If the initial treponemal test is positive and the nontreponemal test is non-reactive, a second treponemal test is completed to establish the diagnosis.
 Fig. 7. Example of quantitative nontreponemal titers that indicated clinically significant change. Source: New York City Department of Health and Mental Hygiene, and New York City STD Prevention Training during pregnancy. Center. Used with permission.
Fig. 7. Example of quantitative nontreponemal titers that indicated clinically significant change. Source: New York City Department of Health and Mental Hygiene, and New York City STD Prevention Training during pregnancy. Center. Used with permission.
Already complicated laboratory interpretation is further complicated by the fact that FTA-ABS testing will be negative in up to 30% of individuals with primary syphilis, leading to missed diagnosis. Alternatives for diagnosis of primary syphilis include dark field microscopy and PCR of a sample collected from the lesion in question. Additionally, even without treatment, nontreponemal titers will decline over time.
6
False positives of both treponemal and nontreponemal tests do occur. False positive tests can occur for many reasons, including pregnancy, advanced age, distant previously treated syphilis infections, connective tissue or autoimmune disorders, other infections, cirrhosis, malignancy, intravenous drug use, some vaccinations, and other endemic treponematosis. In individuals who have previously been treated for syphilis, reinfection is defined by a fourfold increase in a nontreponemal titer.
Cerebrospinal fluid (CSF) analysis is needed for anyone with concerns for neurosyphilis or tertiary syphilis of any kind. CSF analysis should be considered for individuals without neurological symptoms who do not have a fourfold decrease in titers when given an appropriate amount of time, assuming they received stage-appropriate treatment and have not been reinfected.
Repeat lumbar puncture (LP) to confirm successful treatment is not needed if symptoms resolve and serum RPR titer is responding appropriately. The exception is individuals living with AIDS or poorly controlled HIV who need a repeat LP to confirm treatment success even if symptoms resolve. Individuals with ocular syphilis will have a normal CSF analysis 30% to 40% of the time, and those with otosyphilis will have a normal CSF analysis 90% of the time, so confirmatory LP is not necessary.
TREATMENT
Individuals with primary, secondary, and early latent syphilis (infection confirmed less than one year ago) should receive intramuscular penicillin G benzathine 2.4 million units once.
8 Individuals with late latent infection, syphilis of unknown duration, or non-neurologic complications of tertiary syphilis should receive three doses of 2.4 million units of intramuscular penicillin G benzathine at one-week intervals. For non-pregnant patients, intervals can likely be extended up to 10 days without sacrificing efficacy. For non-pregnant, penicillin-allergic patients, doxycycline can be used as an alternative.
Individuals with neuro, ocular, or otosyphilis should be treated with a 10- to 14-day course of continuous intravenous infusion of aqueous crystalline penicillin G for a total of 18-24 million units per day. Alternatives include penicillin G procaine 2.4 million units intramuscularly once daily plus probenecid 500 mg orally four times a day for 10-14 days or daily ceftriaxone infusions.
Pregnant patients must receive penicillin G benzathine. If they need three doses, they must be administered exactly seven days apart or the regimen must be restarted. Penicillin-allergic pregnant patients with syphilis must be admitted to the hospital for desensitization to proceed with proper treatment.
HIGH-RISK GROUPS
Men Who Have Sex with Men
In the 21st century, patients have available to them the proper treatment and diagnostic tools to stop the spread of this disease, but the most vulnerable of patients continue to suffer from syphilis. In 2015, the rates of syphilis in MSM were 167 times higher than in women and 106 times higher than in heterosexual men.
9 The rates of syphilis are highest in PLWHA.
Multiple contributing factors lead to increased syphilis rates among MSM.
8 Anal sex, which is a more common practice among MSM, has a higher likelihood of transmitting sexually transmitted diseases compared to vaginal sex due to increased likelihood for epithelial abrasions and the highly vascular nature of the anus. The practice of serosorting (choosing partners with the same HIV status), which evolved to decrease the rates of transmission of HIV through unprotected sex, has unfortunately increased the rates of syphilis.
Effective treatment for HIV has allowed for the transition of HIV from a deadly disease to a chronic disease, yet has also decreased condom use. Similarly, access to pre-exposure prophylaxis against HIV has increased unprotected sex and STD infections.
8,10,11 HIV infection itself is a risk factor for syphilis.
Having more dense sexual networks, seeking sexual partners through the internet or apps such as Grindr, and increasing drug use with sex are all risk factors for obtaining syphilis which overlap with practices that are more common among MSM.
12 HIV prophylaxis continues to provide an important role in significantly decreasing HIV transmission; it simultaneously provides an opportunity for regular STD testing and treatment.
Pregnant Persons
Unfortunately, with the increased incidence of syphilis comes the rise of syphilis in the pregnant population. A recent study from the National Institutes of Health (NIH) reported a 61% increase in syphilis cases among pregnant women nationally from 2012 to 2016 across all demographics and ethnicities.
13
Pennsylvania is not immune to these statistics. In a recent 2022 Pennsylvania Department of Health advisory, a 36% increase in early syphilis cases in females, of whom 90% were child-bearing age, was reported in the past year.
1 The rise of syphilis in the pregnant population is especially concerning given the high probability for transmission of congenital syphilis to the fetus if left untreated.
14
While the greatest risk of vertical transmission occurs during early syphilis, when disease titers are greatest, syphilis can be transmitted from mother to child at any stage of disease (including latent phases) and during any trimester of pregnancy.
15 Vertical transmission most frequently occurs trans placentally but can also rarely occur during delivery from neonatal contact with a genital lesion.
Congenital syphilis carries significant risks for adverse outcomes, with the World Health Organization estimating that 50% to 80% of pregnancies affected by syphilis end in stillbirth, spontaneous abortion, or other adverse pregnancy outcomes.
14 The fetuses with congenital syphilis that do survive may suffer anemia, blindness, deafness, and hepatosplenomegaly and skeletal abnormalities.
Importantly, the NIH study reporting the rise in syphilis among pregnant women also demonstrated that medical professionals cannot rely on high-risk behaviors to identify women for repeat screening in pregnancy.
13 In the study of 15 suspected risk factors — including high-risk sexual behaviors and drug use — 49% of pregnant women with syphilis did not report any risk factors.
This data and similar reports support the recent Pennsylvania Department of Health advisory that all pregnant patients should be tested for syphilis at the first prenatal visit, the third trimester of pregnancy, and at delivery, regardless of risk factors, ethnicity, age, or socioeconomic status.
1
As up to 80% of pregnant women with untreated syphilis transmit syphilis to their fetus, treatment is of the utmost importance in this population. As stated above, intravenous penicillin G benzathine is the only therapy with confirmed efficacy for syphilis during pregnancy.
PREVENTION
The keys to syphilis prevention are condom use, early diagnosis of infection, and partner treatment. The U.S. Preventive Services Task Force has given a grade A recommendation to screening for syphilis among asymptomatic, non-pregnant adults and adolescents who are at increased risk for syphilis infection.
Doxycycline prophylaxis is an active area of research for syphilis prevention. In a pilot study, 30 MSM living with HIV with prior syphilis infections were randomized to receive either daily doxycycline as pre-exposure prophylaxis (PrEP) for 48 weeks versus a financial incentive-based behavioral intervention.
16 Individuals in the doxy PrEP arm were significantly less likely to test positive for a bacterial STD during the study period compared to individuals in the control arm.
Further, the use of doxycycline post-exposure prophylaxis (PEP) — that is, the use of 200 mg doxycycline within 24-72 hours of unprotected sex among MSM and transgender women — in a 232-participant subgroup analysis in the French IPERGAY cohort resulted in a 70% reduction in chlamydia and a 70-73% relative reduction in chlamydia and syphilis cases.
17
The major and thus far unanswered questions regarding use of doxycycline for PEP and/or PrEP are antimicrobial resistance and microbiome alterations. At this point in time, we recommend rare, and carefully considered, use of doxy PrEP.
CONCLUSION
Syphilis has been present for much, if not all, of recorded history. It is present in Greek mythology, in the tale of the shepherd Syphilus, who angered Apollo.
18 According to the Columbian hypothesis of the origin of syphilis, it was carried from the Old World to the New in the Columbus fleet. It has been a constant companion of war and displacement.
The advent of penicillin in 1928 allowed for treatment of this ever-present but sometimes diagnostically elusive disease. Despite this, syphilis rates are again on the rise nationally and in Pennsylvania, increasing rates of adult morbidity and congenital syphilis. To combat this disease as clinicians, we must screen frequently, take regular and thorough sexual histories, and have a low threshold to include syphilis in our differential diagnosis.
RESOURCES
The National Network of STD Clinical Prevention Training Centers offers an STD Clinical Consultation Network. Consultations can be submitted through
https://www.stdccn.org.
Locally, LGHP Comprehensive Care provides a free walk-in Sexually Transmitted Disease Clinic on Mondays from 4:30-8:00 p.m. where patients can be tested and receive treatment for syphilis.
REFERENCES
1. Pennsylvania Department of Health.
Increases in Reported Early Syphilis. 2022. Health Advisory #625.
2. Daskalakis D. Syphilis: continuing public health and diagnostic challenges.
Curr HIV/AIDS Rep. 2008;5(2):72-77.
3. Division of STD Prevention, National Center for HIV, Viral Hepatitis, STD, and TB Prevention, Centers for Disease Control and Prevention.
Sexually Transmitted Disease Surveillance 2019, Syphilis Surveillance Supplemental Slides, 2015-2019. 2021.
4. Division of STD Prevention, National Center for HIV, Viral Hepatitis, STD, and TB Prevention, Centers for Disease Control and Prevention.
Sexually Transmitted Disease Surveillance 2020, National Overview. 2022.
5. Lake A. LGHP Comprehensive Care providing free STD testing, treatment, and prevention.
Lancaster General Health Clinical Updates. June 2022.
6. New York City Department of Health and Mental Hygiene, and the New York City STD Prevention Training Center.
The Diagnosis and Management of Syphilis: An Update and Review. 2019. Accessed August 4, 2022.
http://www.nycptc.org
7. Lake AC, Kirchner JT. A persistent lip ulcer.
Am Fam Phys. 2018;8(3):185-186.
8. Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021.
MMWR Recomm Rep. 2021;70(4):1-187.
9. de Voux A, Kidd S, Grey JA, et al. State-specific rates of primary and secondary syphilis among men who have sex with men — United States, 2015.
MMWR. 2017;66(13):349-354.
10. Nguyen VK, Greenwald ZR, Trottier H, et al. Incidence of sexually transmitted infections before and after preexposure prophylaxis for HIV.
AIDS. 2018;32(4):523-530.
11. Peterman TA, Su J, Bernstein KT, Weinstock H. Syphilis in the United States: on the rise?
Expert Rev Anti Infect Ther. 2015;13(2):161-168.
12. Schmidt R, Carson PJ, Jansen RJ. Resurgence of syphilis in the United States: an assessment of contributing factors.
Infect Dis (Auckl). 2019;12:1178633719883282.
13. Trivedi S, Williams C, Torrone E, Kidd S. National trends and reported risk factors among pregnant women with syphilis in the United States, 2012-2016.
Obstet Gynecol. 2019;133(1):27-32.
14. Tsai S, Sun MY, Kuller JA, Rhee EHJ, Dotters-Katz S. Syphilis in pregnancy.
Obstet Gynecol Surv. 2019;74(9):557-564.
15. Liew ZQ, Ly V, Olson-Chen C. An old disease on the rise: new approaches to syphilis in pregnancy.
Curr Opin Obstet Gynecol. 2021;33(2):78-85.
16. Bolan RK, Beymer MR, Weiss RE, Flynn RP, Leibowitz AA, Klausner JD. Doxycycline prophylaxis to reduce incident syphilis among HIV-infected men who have sex with men who continue to engage in high-risk sex: a randomized, controlled pilot study.
Sex Transm Dis. 2015;42(2):98-103.
17. Molina JM, Charreau I, Chidiac C, et al.; ANRS IPERGAY Study Group. Post-exposure prophylaxis with doxycycline to prevent sexually transmitted infections in men who have sex with men: an open-label randomised substudy of the ANRS IPERGAY trial.
Lancet Infect Dis. 2018;8(3):308-317.
18. Tampa M, Sarbu I, Matei C, Benea V, Georgescu SR. Brief history of syphilis.
J Med Life. 2014;7(1):4-10.