Fall 2019 - Vol. 14, No. 3

PHOTO QUIZ FROM URGENT CARE
A Woman with Ear Pain
Rodney Hostetter, PA-C
Penn Medicine Lancaster General Health Urgent Care
CASE HISTORY
A 46-year-old female presented with two to three days of right external ear pain, without fever or headache. She denied feeling pain deeper in the ear area. She had no history of similar ear pain or recent ear infection.
Examination revealed mild erythema, swelling, and tenderness of the middle of the external ear (Fig. 1). There was no fluctuance. The ear canal and tympanic membrane were both normal. She had no erythema, swelling, or tenderness of the mastoid or the face, and no other area of redness or rash on the head.
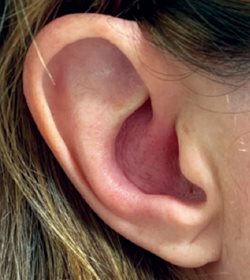
Fig. 1. Patient with perichondritis, an infection of the middle of the external ear.
QUESTIONS
1. Which bacteria are the most common cause of this type of infection?
2. What are the most common risk factors for developing this infection?
3. Which long-term complication can occur if this problem is not treated appropriately?
4. What features of this infection would prompt an immediate specialty or hospital consultation?
5. How would treatment change if this were an infection of the ear lobe instead of the auricle?
ANSWERS
1. Pseudomonas Aeruginosa is the most common causative organism in cases of perichondritis.
2. The most common risk factors are trauma (increasingly cartilage piercing and acupuncture), recent surgery, and burns, although none were present in this case.
3. Liquefying chondritis is a complication that can result in permanent deformation of the auricle.
4. Signs of abscess or necrosis should prompt an immediate specialty or hospital consultation.
5. Perichondritis spares the ear lobe (Fig. 2). Fluoroquinolones are the antibiotic of choice for outpatient treatment of perichondritis, but an infection of the ear lobe is more prudently treated with a non-fluoroquinolone antibiotic.
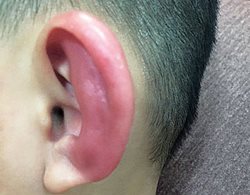
Fig. 2. For comparison: A picture on the National Institutes of Health website shows
an advanced case of perichondritis with sparing of the ear lobe.
DISCUSSION
Perichondritis is an infection of the cartilaginous auricle or pinna, often, but not always, precipitated by trauma. Inaccurate treatment is not uncommon, due to incorrect antibiotic choice (Fig. 2). The treatment of perichondritis differs from treating simple cellulitis, where the likely causative organisms are streptococcus or staphylococcus. In the majority of perichondritis infections, the causative organism is Pseudomonas aeruginosa, and antibiotic therapy should be tailored accordingly. For inpatient management there are a number of antibiotics to choose from, but for outpatient management (mild to moderate infections that do not include abscess or necrosis) a fluoroquinolone antibiotic should be prescribed.
REFERENCES
1. Pescatore R. Perichondritis: Not Just Simple Cellulitis.
RebelEM. 2017
https://rebelem.com/perichondritis-not-just-simple-cellulitis/
2. Davidi E, Paz A, Duchman H, Luntz M, et al. Perichondritis of the auricle: analysis of 114 cases.
Isr Med Assoc J. 2011; 13(1):21-4
3. Kanj SS, Sexton DJ. Pseudomonas aeruginosa infections of the eye, ear, urinary tract, gastrointestinal tract, and central nervous system.
UpToDate. Literature review current through July 2019.
https://www.uptodate.com/contents/pseudomonas-aeruginosa-infections-of-the-eye-ear-urinary-tract-gastrointestinal-tract-and-central-nervous-system
4. Saxena SD, Splanger M. (2019). Perichondritis.
J Urg Care Med. Online at:
https://www.jucm.com/perichondritis/