Winter 2018 - Vol. 13, No. 4

PHOTO QUIZ FROM URGENT CARE
Monkey Bars, Monkey Business
Dustin L. Yothers, MSPAS, PA-C
Penn Medicine Lancaster General Health Urgent Care
CASE HISTORY
A young girl fell off monkey bars in the schoolyard. She did not lose consciousness, and was taken directly to Urgent Care after her mother was notified. Her fall had not been observed by her teacher or classmates, but she said that she had landed directly on her left elbow. She complained of left elbow pain without numbness or tingling, but not of any other injuries or pain.
She was tearful, and used her right hand to hold her left elbow at a 45-degree angle for comfort and support. There was no tenderness over her left shoulder or wrist, and no abrasions or lacerations elsewhere on her body. Plain film radiographs of her left elbow were ordered (Fig. 1, a & b).
QUESTIONS
1. What types of injury should be suspected prior to viewing the films?
2. What fracture is revealed by the X-ray?
3. Based on the X-ray findings, what type of splint should be used?
4. Is this an orthopedic emergency?
5. What is the treatment approach?
6. What are the most common long-term complications?
ANSWERS
1. Elbow dislocation, supracondylar fracture of the humerus, radial head fracture, olecranon fracture, lateral condyle fracture, Monteggia fracture; also consider associated clavicle, shoulder, and/or forearm and wrist fractures.
2. Acute, mildly displaced Type III supracondylar fracture with dorsal angulation of the distal humerus and associated joint effusion. (See below for further discussion of fracture types.)
3. A posterior long arm splint with the elbow flexed at approximately a 75-90
o angle, with a sling. The splint should be placed without compromising neurovascular status and with appropriate pain management that prevents too much discomfort. Distal pulses should be checked before and after placing the splint. If deformity is noted on the initial exam, it is important to place a splint prior to obtaining X-rays.
4. This is not an open fracture, nor is there neurovascular compromise or evidence of compartment syndrome, which would be obvious emergencies.
5. The urgency in this case is less obvious, but it is a Type III fracture with mild displacement. After splinting, it warrants referral to the Emergency Room where orthopedic consultation will be available. Alternatively, if an immediate evaluation can be guaranteed at an orthopedic office, this would also be acceptable.
In the interest of communicating comprehensively with the parents, it is well to mention the possibility that surgery might be needed, however the details of the surgery should be left for the surgeon to discuss.
6. Vascular insufficiency, forearm compartment syndrome resulting in Volkmann’s ischemic contracture, nerve injury, and cubitus varus deformity, are among some of the most common long-term complications seen with supracondylar fractures of the humerus.
DISCUSSION
This case demonstrates a supracondylar fracture of the humerus. These fractures are common in children, and account for approximately 60% of elbow fractures, because the supracondylar region is composed of thin, weak bone, particularly in the distal posterior humerus.
1 The most common causes are direct trauma or a fall on an outstretched hand (FOOSH), most commonly on the non-dominant side.
These fractures are classified according to the Gartland classification system: type I, type II, and type III. In the simplest terms, type I is non-displaced, type II is displaced with an intact posterior periosteum and cortical continuity, and type III is displaced with disrupted anterior and posterior periosteum and lack of cortical continuity.
2 This fracture is a type III because the AP projection shows lateral displacement. This could only occur if both the anterior and posterior cortices are broken.
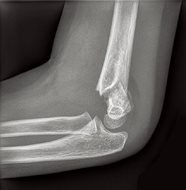
Fig. 1a: Lateral view of left elbow.
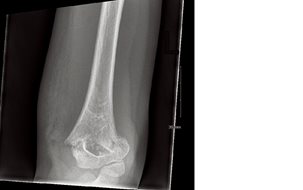
Fig. 1b: AP view of elbow.
Clinical findings in these fractures include: elbow pain, swelling, bruising, and a very limited range of motion. Rapid assessment is crucial as there may be neurovascular compromise involving the median nerve and brachial artery. Examination should focus on evidence of compartment syndrome or injury to radial, medial, and ulnar nerves, with attention to pulses, capillary refill, and two-point discrimination.
3 The joints above and below the elbow should be examined carefully, as many of these fractures are associated with secondary fractures. An obvious deformity of the elbow warrants splinting before imaging, with adequate analgesia for the level of the patient’s discomfort.
Immediate orthopedic consultation should be obtained if there is an open fracture, a fracture with neurovascular compromise, a type II or III supracondylar fracture, and/or evidence of compartment syndrome.
4 Without prompt, appropriate treatment, these patients could develop vascular insufficiency, forearm compartment syndrome resulting in Volkmann’s ischemic contracture, nerve injury, and cubitus varus deformity, which are among some of the most common long-term complications seen with supracondylar fractures of the humerus.
5
If the exact type of supracondylar humerus fracture is not known, or if there is any concern for pain out of proportion to the injury, do not hesitate to splint and send immediately to the emergency department or call directly to an orthopedic practice for advice. An unnecessary immediate referral is much better than risking a devastating complication due to delay in treatment.
If the patient has a type II or type III fracture, they are more likely to end up needing surgery. The usual procedure is open or closed reduction and percutaneous pinning, followed by placement in a splint or cast. The pins will be removed once there is good evidence of bony healing seen on X-rays, typically 3-4 weeks. Most patients do not require physical therapy.
6
Overall, these fractures often have a good prognosis despite common immediate complications. Most complications (~1%) are either self-limited or corrected with surgical intervention.
7
REFERENCES
1. Houshian S, Mehdi B, Larsen MS. The epidemiology of elbow fracture in children: analysis of 355 fractures, with special reference to supracondylar humerus fractures.
J Orthop Sci. 2001; 6(4): 312-315.
2. Alton TB, Werner SE, Gee AO. Classifications in brief: the Gartland classification of supracondylar humerus fractures. Clin Orthop Relat Res. 2015;473(2):738-41. doi: 10.1007/s11999-014-4033-8.
3. Garg S, Weller A, Larson AN, Fletcher ND, et al. Clinical characteristics of severe supracondylar humerus fractures in children.
J Ped Orthop. 2014; 34(1): 34-39.
4. Oetgen ME, Mirick GE, Atwater L, et al. Complications and predictors of need for return to the operating room in the treatment of supracondylar humerus fractures in children.
Open Orthop J. 2015; 9(5): 139-142.
5. Omid R, Choi PD, Skaggs DL. Supracondylar humeral fractures in children.
JBJS; 2008; 90(5): 1121-1132.
6. Acar E, Memik R. Surgical Treatment Results in Pediatric Supracondylar Humerus Fractures. Eurasian
J Emerg Med 2017: DOI: 10.5152/eajem.2017.74046
7. de Neira JZS, Prada-Cañizare A, Marti-Ciruelos R, et al. Supracondylar humeral fractures in children: current concepts for management and prognosis.
Internat orthopaedics. 2017; 39(11): 2287-2296.